TMJ/TMD from Ramin Mehregan
Ramin Mehregan D.M.D.
Friday, December 19, 2014
Thursday, November 6, 2014
Saturday, October 25, 2014
DIET FOR TMD (Temporomandibular Dysfunction)
Does This Sound Familiar?
"My jaw hurts and feels tired when I eat!"
"My jaw makes loud noises when I eat!"
Temporomandibular joint and muscle disorders involve the chewing muscles and joints connecting the lower jaw to the skull. Although TMJ is technically the abbreviation for the joint, people commonly use this term as shorthand for the disorders and symptoms.
The TMJ's:
The temporomandibular joints are located on each side of your head in front of your ears, connecting your lower jaw to your skull. A small cartilage disc separates the bones so the lower jaw slides easily. You move these joints every time you chew, swallow and talk, so they are used very frequently.
Symptoms:
Symptoms of TMJ can include jaw discomfort and tenderness or pain when opening or closing the mouth. You may find it uncomfortable to chew, or there may be popping or grating sounds when you move your jaw. TMJ can cause headaches, earaches, facial pain and neck, shoulder and back pain. Symptoms can be caused or worsened by physical stress on structures around the joint, poor posture, neck and facial muscle strain, lack of sleep, life stress and poor diet.
The right diet is part of the treatment:
To lessen pain and other symptoms avoid eating hard foods, crunchy foods, thick or large foods that involve opening your mouth wide and foods that require a lot of chewing. This gives your jaw and temporomandibular joints the opportunity to rest.
The Nutrition:
1) Eat a good balanced diet to protect your TMJoints:
- Place yourself on soft diet (I don't mean liquid), which would consist of foods such as cooked vegetables, eggs, ground meat, fruits, etc.
- Avoid biting into a whole apple, corn on the cob, large pieces of lettuce in your salad, large pieces of meat, chewy snacks such as chips, and ice.
- For you chewing gum lovers out there......that is a definite "NO".
- By cutting down your food into small bite size pieces, you can reduce the stress to your chewing muscles and joints. And eat slower.......hmmmmm isn't that what our mother's used to tell us????
- NutraSweet
- Chocolate
- Alcohol
- Caffeine
- Nicotine
- Sugar (yes that includes the old soda pop)
- Excessive dairy products
- Excessive salt (use sea salt)
- Whole Nuts
- Water (how much??????)
- Fresh fruits
- Fresh vegetables
- Greens (Kale, Spinach, etc)
- Whole grains (cereal, breads, etc)
- Chicken, fish, tender beef
- Complex carbohydrates such as sweet potatoes
- Herbal teas
- Almond/Soy Milk
- Greek yogurt (not those fruity sweetened stuff....add you own fruit and honey)
- Healthy, energy boosting smoothies
- Some great links to healthy food and smoothie recipes that I frequent a lot:
- http://simplegreensmoothies.com/
- http://kblog.lunchboxbunch.com/
- http://www.inspirelearnlive.com/50-natural-energy-boosting-smoothie/
- http://www.topinspired.com/top-10-healthy-food-recipes/
Enjoy!
Monday, April 21, 2014
Listening To And Learning From YOU!
Is listening part of your practice culture?
A CRITICAL COMPONENT of personalized patient care is cultivating the art of listening. Listening is key to all communication, without the ability to listen effectively messages are easily misunderstood - communication breaks down and the sender of the message can easily become frustrated or irritated.
Listening is not the same as hearing!
Being privileged to be a part of few TMJD discussion group forums, I frequently encounter posts like the following:
"I have found solution to my TMD and facial pain in meditation. I need to do more meditation to find the doctor. The doctor who listens and grasps the essence."
"My doctor says I am imagining my symptoms...because of the symptoms that comes with TMJ, I have stress and anxiety. It's awful and definitely not imagined!"
"Some doctors will prescribe anti-depressants and anti-anxiety meds because they think it is mental..."
"Some doctors will prescribe anti-depressants and anti-anxiety meds because they think it is mental..."
"If a patient is following YOUR protocol....and has raised acute pain from your splints/orthotics....something is NOT right!! Please doctors don't blame the patient for non compliance. We are the ones that have to try and wear these (at times non measured) appliances.....and are in agony....not you....For the love of all that is good in this universe....please listen to your patients!!!"
"...please, oh please don't tell your patient that they are just stressed and need to relax. Anxiety and depression can be a factor in the process, but It isn't an excuse when you are having trouble helping your patient."
"...we become our own doctors when it comes to tmj so plllllease listen to your patient you never know it might help them.."
"Well that was a waste of time. He didn't even examine me, nor give me vitamin D. Spent 30 minutes saying it was all psychosomatic & that he didn't believe teeth could ever cause such problems."
"I am currently in severe headache with TMJ. God Please Help me. meds are useless and my doc keeps prescribing them to me....he doesn't get it..."
"I have been dealing with TMJ and ear problems for about 7 years. I've been to so many doctors and they all have different opinions and only hear themselves. I think they are all full of themselves..."
Unfortunately I could go on with these type of comments, and it saddens me to see so many professionals lacking the ability of effective listening.
Listening is not the same as hearing and in order to listen effectively you need to use more than just your ears.
The 5 Principles of Listening
A good listener will listen not only to what is being said, but also to what is left unsaid or only partially said.
Effective listening involves observing body language and noticing inconsistencies between verbal and non-verbal messages.
1. Undivided Attention
- Open communication through active listening is the keystone of good health care. Active listening is a therapeutic technique that establishes trust in a health care professional-patient relationship. To begin, give the patient your undivided attention and refrain from interrupting until he is finished speaking. Ignore distracting thoughts and avoid outside distractions, including environmental factors and other people's conversations. Focus on the person to show he has your undivided attention.
2. Body Language
- Body language is just as important as what you say during a conversation. Maintain eye contact and nod at appropriate times to show you are actively engaged in what your patient has to say. Avoid crossing your arms and keep an open posture to show you are open to communication. Avoid grimaces and frowns, which can discourage patients from sharing personal information due to embarrassment. Oftentimes, patients are already scared and uncomfortable when coming to an office or medical facility. By simply touching her hand, you can encourage her to share more details about her condition.
3. Acknowledgement
- After listening to what your patient has to say, paraphrase her comments to verify your understanding of the situation. Not only will this clear up any misconceptions you have, but it also helps to validate the patient's feelings about what she is going through. Clarify important details by asking if you have a thorough understanding of what he is saying and feeling. Ask open-ended questions to help him elaborate on key aspects you want to take note of or record in his chart. As an active listener, the most important goal is to understand what your patient is saying.
4. Nonjudgmental Attitude
- Once you have a thorough understanding of your patient's message, withhold judgment, even if you disagree. Avoid interrupting with counterarguments, which stifle conversation and can ruin trust. Critical comments will only frustrate the patient and limit your understanding of his message. As a medical professional, it is your job to provide care and understanding without judgment of your patient's choices and experiences.
5. Response
- Active listening is based on honesty, trust and understanding. Provide your professional opinion of the situation, but don't talk down to the patient just because she doesn't have the same medical training as you have. By clarifying the patient's message, you can help him explore other points of view. Show your empathy for the patient by treating her with respect. Always treat patients the way you would want to be treated if the situation were reversed.
Friday, April 18, 2014
Ways Laughter And A Confident Smile Are Life Changing
"You don't stop laughing because you grow old. You grow old because you stop laughing."
BECAUSE IT USUALLY HAPPENS SPONTANEOUSLY, we don’t often think about smiling or laughing. However, they both really do make us feel better—and, studies continue to reveal more of their many benefits.
 It boosts your immune system:
It boosts your immune system:
Smiling really can improve your physical health, too. Your body is more relaxed when you smile, which contributes to good health and a stronger immune system.
 Smiles are contagious:
Smiles are contagious:
It’s not just a saying: smiling really is contagious, scientists say. In a study conducted in Sweden, people had difficulty frowning when they looked at other subjects who were smiling, and their muscles twitched into smiles all on their own.
 Smiles relieve stress:
Smiles relieve stress:
Your body immediately releases endorphins when you smile, even when you force it. This sudden change in mood will help you feel better and release stress.
 Forcing yourself to smile boosts your mood:
Forcing yourself to smile boosts your mood:
Psychologists have found that even if you’re in bad mood, you can instantly lift your spirits by forcing yourself to smile.
 It's easier to smile than to frown:
It's easier to smile than to frown:
Scientists have discovered that your body has to work harder and use more muscles to frown than it does to smile.
 Smiling lifts your spirit and those around you:
Smiling lifts your spirit and those around you:
Life is full of ups and downs. Smiling can reduce distressing emotions and be an invaluable tool in moving forward with our heads held high. And equally important, grins and chuckles can calm and comfort those around us. Here’s an example of how someone else’s smile (laugh) can lift YOUR day… I dare you to watch this video without smiling:
 Smiles are exercises for your facial muscles:
Smiles are exercises for your facial muscles:
53 muscles are used when you smile. Other smiles can take up to 5 muscles. So start working those muscles more often!
 Babies are born with the ability to smile:
Babies are born with the ability to smile:
Babies learn a lot of behaviors and sounds from watching the people around them, but scientists believe that all babies are born with the ability, since even blind babies smile.
 Smiling helps you get promoted:
Smiling helps you get promoted:
Smiles make a person seem more attractive, sociable and confident, and people who smile more are more likely to get a promotion.
 Smiling fights stress:
Smiling fights stress:
If you're feeling burnt out and tired of the routine, just smile. When you smile, your body releases endorphins (aka “Happy Hormones”), even if it’s a fake smile, this sudden mood change will relieve stress.
 Smiling makes you look really pretty:
Smiling makes you look really pretty:
Who needs makeup when you have this secret ingredient to instant glam? A research study by Orbit Complete revealed that 69% of people find women who smile more attractive than women who wear a lot of makeup.
 Smiling may help you look younger:
Smiling may help you look younger:
That elusive fountain of youth may not be found in surgeries or potions—rather, a study suggests that the path to looking younger may be found through our smiles.
Mark Twain once wrote, “Wrinkles should merely indicate where smiles have been!” The act of smiling is a very uncomplicated and important human activity. It really isn’t important that your smile be perfect- but that you feel good about it and you give it away! If your stingy with your smile because it’s something less than what you want it to be, I can help – Smiles are the best that you can put on!
Sunday, December 29, 2013
THE VICIOUS CYCLE OF TEMPORO-MANDIBULAR-JOINT DYSFUNCTION
The Vicious Cycle of TMJD,
And How It Affects Its Treatment
Temporomandibular Joint Dysfunction (TMJD) arises when the harmony of teeth, facial muscles, and the temporomandibular joints no longer exist. Some of the clinical symptoms are:
- Headaches
- Neck and shoulder aches
- Ringing in the ears and ear congestion
- Clenching/grinding
- Limited opening/movement of the lower jaw
- Dizziness/vertigo
- Clicking/popping of the jaw joints
The Vicious Cycle
TMJD is a chronic degenerative disease which often takes years to develop. There are many contributing factors that if not diagnosed can and will affect the outcome of its treatment. Every person/patient has a unique personality and biological make-up, and it must be considered when discussing cause and treatment of TMJD.
The three factors affecting treatment and consequently the outcome are:
- Structural
- Emotional
- Biochemical
A person suffering from TMJD is affected by these three factors in some shape and form and seldom to an equal extent. Hence, it is fundamental when diagnosing TMJD, to asses the relative impact of each of these factors. Many patients may remain oblivious of any symptoms until one day they wake up with, for example an excruciating headache. It is like filling a cup of water to the rim and one keeps adding droplets until all of the sudden there is a spill over. Similarly, many different lifestyles can combine which could aggravate TMJD - such as structural imbalance, stress, depression, fatigue, nutrition and even simply routine check up visits to the dentist. Any of these are like "the single drop" in the cup of water.
Structural
One of the primary root component that is always present in TMJD is structural imbalance. Structural Imbalance. We often hear this phrase used along with the diagnosis of our aches and pains. But what does it mean? The best way to explain it is to start from the opposite end, "Structural Balance".
Structural Balance refers to the optimal positioning of our bones and joints. This means when weight or pressure is applied to a part of the body, it is effectively passed through the structures, e.g. bones, joints and muscles. These structures are designed to hold weight well in a particular direction and not so great in other directions. Structural imbalance is simply when bones, joints and muscles are not in their optimal position when weight and pressure is applied.
In the presence of mal-occlusion the skeletal system is in disharmony with neuromuscular system. This means that the teeth/occlusion is forcing the TMJoint's and muscles into a strained position. The aforementioned state increases the natural demand to the muscle and nervous system beyond their natural biological capacity and places them in a spasm cycle.
It is just like walking with a pebble inside your shoe. After a few yards the pain becomes annoying and will twist and torque your hip into all kind of different positions to avoid walking on the pebble inside your shoe (this manipulation is known as accommodation/avoidance). After few more painful steps the pebble will start to feel like a large stone and your foot, leg and body is left in tremendous agony and distress. The former metaphor can be related to what happens to the muscles of the face and jaw (oro-facial muscles) when they are forced into an unnatural position by virtue of a "bad bite". Eventually the muscles become strained and painful. This strain on the muscles causes an alteration in their shape and tonus. To compensate for this the other muscles such as the neck, shoulder and back have to accommodate for this unnatural position, which in turn places them into a strain and spasm.
"Muscles under constant strain are in pain"
Emotional
Many medical/dental professionals are still of the opinion that TMJD is a psyhosomatic (psych=mind, soma=body) illness, starting in the mind and manifesting itself in the body. Sometimes humans continually complain of a discomfort or a pain for which a health professional cannot find an organic cause. The pain or the discomfort, however, is very real to the affected person. Physical complaints with no apparent medical basis may be a reflection of a stress in social settings, relationships, work environment and or other stressful situations for example. Stress, as it affects the body and the mind, has an effect on some illnesses, such high blood pressure, ulcers, and can influence as how humans perceive the symptoms of the illness, how he or she deals with the illness, and the rate and success of recovery.
It is believed, however, that for most part TMJD has its origin from a structural imbalance or "somatopsychic". The resulting pain in the muscles (soma) causes a feeling of anxiety, tension and stress (psyche). There have been numerous studies on how the impact of being sick affects us mentally and emotionally. For instance emotional reactions when having a daily headache could include:
- Inability to perform up to ones personal and public expectations
- Anxiety
- Depression
- Frustration
- Lack of energy
- Anger and hyper-irritability
- Fear of the unknown
"My silence is just another word for My pain"
Biochemical
The human body and mind has certain arsenal to its possession when in pain and in stress. In pursuance of pain and stress it prepares itself for either "fight or flight". These are short term positive coping mechanism in the presence of stress. Unfortunately when in pain, under stress and emotional constraints at the same time, we tend to add to the problems by adopting less favorable habits such as:
- Over-eating
- Drug and alcohol consumption
- Medications - prescribed and non prescribed
- Sleeplessness
- Not exercising
Soon the body adapts itself to long term chronic stress. In this second stage, the body's defense hormones operate in an above-normal rate. In addition to the aforementioned ill-habits, just like your car would eventually run out of fuel, the body will soon be depleted from its natural fuel supply. At the third stage, exhaustion sets in and the body breaks down. This stage makes it very difficult to treat a chronic disease such as TMJD. The astute clinician treating TMJD may be successful in properly aligning the structural imbalances but some deep seated emotional and bio-chemical disorders need to be managed by appropriate experts or the treatment will fail.
With TMJD the body is placed in constant stress. The extent and severity differs from individual to individual. Some people may have an occasional click in their TMJoints and some some may suffer from constant, severe, daily pain. In either case, the body prepares itself to fight against the stressor. Biochemical changes occur to provide the body with energy to compensate and adapt. This energy is limited however, and eventually will be depleted at a faster rate, especially in the presence of ill-habits and some emotional conditions. This in turn will affect the success of treatment and its longevity. It is of utmost importance that the treating clinician has the ability to recognize the biochemical and emotional factors of their patient and through discovery and co-communication plan for a successful treatment.
"It is important to know the person who has the disease as to know the disease the person has."
Monday, November 18, 2013
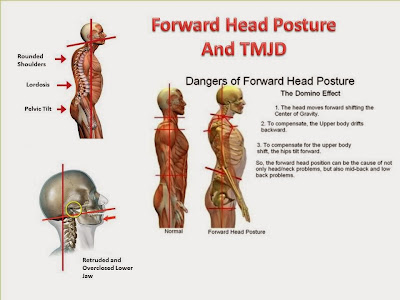
THE 40 POUND HEAD - DAMAGING EFFECTS OF FORWARD HEAD POSTURE
Forward head posture and its effects on health and the craniomandibular complex
The effect of posture on health is becoming more evident. “Spinal pain, headache, cranio-mandibular-joint effects, mood, blood pressure, pulse and lung capacity are among the functions most easily influenced by posture.
One of the most common postural problems is the forward head posture (FHP). Since we live in a forward facing world, the repetitive use of computers, TV, video games, trauma, compromised occlusal plane and even backpacks have forced the body to adapt to a forward head posture. It is the repetition of forward head movements combined with poor ergonomic postures and/or trauma that causes the body to adapt to forward head posture.
A review of literature substantiates that "For every inch of forward head posture, it can increase the weight of the head by and additional 10 pounds." It's not uncommon to have TMD patients walk into my office supporting a 10-12 lb head that has migrated 3 inches forward of their shoulders. It isn't difficult to recognize prior to any palpation that their cervical muscles are in a losing battle attempting to isometrically restrain 40-42 pounds against the unrelenting forces of gravity.
Ideally, the head should sit directly on the neck and shoulders, like a golf ball sits on a tee. The
weight of the head is more like a bowling ball than a golf ball, so holding it forward, out of alignment, puts a strain on your neck and upper back muscles. The result can be muscle fatigue and all to often an aching neck. Head forward posture can add up to thirty pounds of abnormal leverage on the cervical spine. This can pull the entire spine out of alignment.
Because the neck and shoulders have to carry this weight all day is an isometric contraction, this causes neck muscles to loose blood , get damaged, fatigue, strain, cause pain, burning and fibromyalgia. When spinal tissues are subject to a significant load for a sustained period of time,
they deform and undergo remodeling changes that could become permanent.
It also has been noted that forward head posture
may result in the loss of 30% of vital lung capacity.
These breath related effects are primarily due to the
loss of the cervical lordosis which blocks the action of the
hyoid muscles, especially the inferior hyoid responsible for helping the first rib during inhalation. Proper rib lifting action by the hyoids and anterior scalenes is essential for complete aeration of the lungs.
Head Posture and Cranio-mandibular posture
The relationship of the mandible to the cranio-maxillary complex, the temporomandibular joints, the atlas and the cervical and thoracic vertebrae are orthopedic in nature. In addition the shoulders, clavicles and sternum are all affected during the action of mastication and swallowing. Many of theses structure either share the same neuro-muscular system or have close commonalities.
Patients with deep bites, retruded lower jaws (Class II mal-occlusion), deficient vertical dimension, narrow introral arches typically present with a forward head posture and a variety of symptoms related to TMJD.
Often seen as a structurally subtle body segment, the neck is burdened with challenging task of supporting and moving the human head. Because of tension and poor postural relationship of the craniomandibular complex and habits inherent in today's workplace and society it comes as no surprise that associated neuromuscular disorders rank high as the most common pain generators. Correction of the upper cervical area and the mandibular relation to the cranio-maxillary complex is key to stoping and reversing degenerative joint disease and pain from headaches, breathing abnormalities, TMJ dysfunction and other postural effects. Any loss of function sets off reactions within the body's open, dynamic system which manifests as structural abnormalities throughout the entire body.
Subscribe to:
Posts (Atom)